- Home
- Mind & body
- A quick guide to chemotherapy
At CBHS we help you manage your health challenges. We believe in offering you the services, support and tools you need to live your best life.
Health and Wellness Programs are available to support eligible members towards a healthier lifestyle. Each Health and Wellness Program is subject to its own eligibility criteria.
Contact us for more information and to confirm your eligibility for a program.
A quick guide to chemotherapy

A brief introduction
Did you know, someone is Australia is diagnosed with cancer every four minutes? The disease is characterised by abnormal cells that grow and reproduce quickly and at an uncontrollable rate. Chemotherapy is one of the main treatments.
How does it work to control the disease?
Chemotherapy uses drugs to destroy abnormal cells that are rapidly dividing. Cancer cells generally grow faster and divide more quickly than normal cells, so chemotherapy works to kill more cancer cells than healthy cells.
Most normal cells in the human body don’t divide unless they are damaged and need repair, but there are exceptions. Some cells (like those in our hair) regularly divide and chemotherapy drugs can also kill rapidly dividing normal cells. So if you need to have chemotherapy you may lose your hair. Thankfully, normal cells can generally repair and recover once your treatment is over (unlike cancer cells).
What sort of drugs are used?
There are around 100 different chemotherapy drugs available and these are known as cytotoxic drugs. Each of these work in a slightly differently way. Some drugs might interfere with the genetic make-up of cells, others might block access to the nutrients that cells need to divide and multiply.
Depending on the type of cancer you may have, and how far it might have spread, it’s not unusual for a combination of drugs to be used to improve your chances of a successful course of treatment. An oncologist (cancer specialist) can advise you on the most suitable form of treatment.
“Chemotherapy can be used on its own or in conjunction with other treatments including, surgery or radiotherapy.”
How do I receive chemotherapy?
Chemotherapy can be delivered in a number of ways including:
- Intravenously as liquid through a thin tube into a vein
- Orally by swallowing tablets or capsules
- Direct injection or topically e.g., by using a cream for skin cancer.
The most common way to have chemotherapy treatment is intravenously (through a drip) in hospital. This is usually as an outpatient service. However, it is possible to have some chemotherapy treatments through a portable pump that you can use at home. Chemo@home, one of our chemotherapy at home providers reports that one of the benefits to having chemotherapy at home is that there is less risk of developing a fever or an infection while white blood cell count is low.
Chemotherapy drugs are powerful, so if you’re taking them at home you should always keep them in a safe, secure place and out of reach of children. People without cancer should avoid direct contact with cytotoxic drugs. So if you’re receiving chemotherapy, talk to your treatment team about any further precautions you might need to take at home.
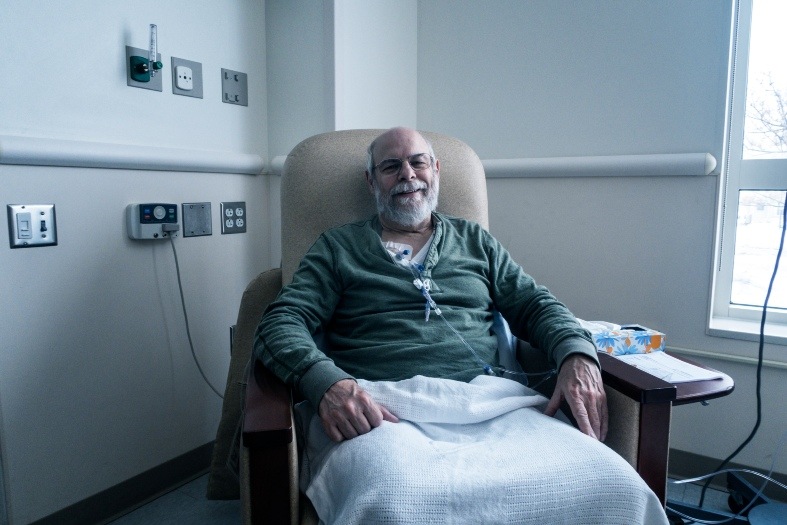
Is chemotherapy successful?
Chemotherapy is often used in conjunction with other forms of treatment, so it’s hard for researchers to provide success rates for chemotherapy alone.
Successful treatment rates for various forms of cancer treatment have increased in the past three decades. Figures from 30 years ago show five in 10 people survived for at least five years after a cancer diagnosis.
“Based on recent recovery rate studies, 7 in 10 people now survive for several years after a cancer diagnosis.”
Chemotherapy can be used for a variety of reasons:
- To cure cancer. Doctors often call this remission, rather than cure. This means signs or symptoms of cancer are no longer present.
- To support other treatments. Chemotherapy can shrink tumours which in turn can help make other treatments, such as surgery, more effective.
- To control cancer. In cases where chemotherapy can’t achieve a ‘cure’ it may control the growth and spread of a cancer.
- To relieve symptoms. Chemotherapy can improve quality of life by shrinking a cancer that causes pain or other symptoms.
- To prevent cancer coming back. Maintenance chemotherapy, sometimes given with other drug therapies, aims to prevent or delay cancer returning.
How long does treatment last?
A course of chemotherapy treatment is usually given in cycles, to allow periods of rest in between treatments. This gives healthy cells time to recover. A single session of chemotherapy given via a drip can take just 20 minutes or up to several hours.
Treatments might be delivered every 3-4 weeks, although each treatment plan differs depending on the individual. A full course of treatment can last between three and six months. Although, the time period is determined by the severity of the symptoms and a specialist’s guidance. For instance, maintenance or palliative chemotherapy can continue for months or in some cases years.
Why does chemotherapy cause side effects?
Side effects are a direct result of damage caused to healthy cells in the body. You may experience these effects at some point during your treatment.
Chemotherapy drugs that circulate in the bloodstream can reach abnormal cells almost anywhere in the body. The drugs work by targeting cells as they divide and, since cancer cells divide faster and more often than normal cells, chemotherapy is more likely to find and kill them.
Most normal cells in our bodies aren’t as active as cancer cells. They only divide if they’re damaged and need to repair. However, some cells such as those in hair, nails, bone marrow, skin and the lining of our digestive system are constantly growing and dividing. This is why chemotherapy drugs can damage these cells.
“A full course of chemotherapy can last between three and six months or for a time period determined by symptoms and a specialist’s advice.”
What are the most common side effects?
There are over 100 different chemotherapy drugs and different drugs cause different side effects. It’s important to remember that you’re unlikely to experience every side effect listed here:
- fatigue, loss of appetite, nausea and bowel changes such as constipation or diarrhoea
- anaemia, hair loss, bleeding problems, mouth sores, dry eyes, skin and nail problems
- trouble concentrating or forgetfulness
- reduced levels of white blood cells which can lead to an increased risk of infection
- chemotherapy can also have an impact on sexuality and fertility.
Medication can reduce the impact of some side effects such as pain and nausea – but it can differ from person to person.
Sometimes chemotherapy can cause long term issues such as infertility and damage to the heart, kidneys, liver, lungs or brain. Speak to your oncologist if you want to have children in the future, so you can discuss your options before you start treatment.
Many side effects can be managed or treated. The good news is that most will go away on their own once your treatment has finished. Another important thing to note here is that side effects are not related to the success of chemotherapy treatment.

How to manage side effects
Some people keep a diary to record specific details of any side effects they experience. They may choose to note how long the effects lasted as well as anything that helped alleviate them.
Most side effects (such as hair loss) are temporary and the damage is usually short-term. Normal cells can generally repair or replace cells damaged by chemotherapy once the drug treatment is complete.
“Your CBHS Hospital cover may give you access to a home-based cancer support program with psychologists, dietitians and more.”
Can you combine exercise with chemotherapy?
If you believe that gentle physical movement will help you during your treatment, and you’ve spoken with your specialist, then yes, by all means. In fact, many cancer organisations are calling for exercise to be prescribed to all people with cancer as part of their routine cancer care.
According to the Cancer Council, only one in ten people diagnosed with cancer will get enough exercise during or after their treatment. However, research has shown that people with cancer who exercise regularly have fewer and less severe side effects. Exercise can also counteract fatigue.
Of course, it’s important to remember that, exercise should be appropriately prescribed and monitored if you’re having chemotherapy treatment. That’s why it’s a good idea to speak with your oncologist before starting a new exercise routine.
Can you have chemotherapy when you’re pregnant?
Firstly, a cancer diagnosis during pregnancy is rare. In fact, the Cancer Council estimates only one in every 1,000 women is affected by the disease.
Chemotherapy during the first 12 weeks of pregnancy may increase the risk of miscarriage or birth defects as well as potentially cause premature delivery. The drugs can also affect sperm, so, if possible, you and your partner should avoid falling pregnant during chemotherapy treatments. Experts also don’t recommend breastfeeding during chemotherapy because the drugs can be passed to your baby through breastmilk.
If you are pregnant when you’re diagnosed, reach out to your specialist for advice and guidance on the best treatment options available to you.
“Light, regular exercise during chemotherapy treatment can counteract fatigue and reduce the severity of side effects.”
Is chemotherapy covered by my health insurance?
Depending on your policy and your level of Hospital cover, some chemotherapy treatments are covered by health insurance. Log into your Member Centre or mobile app to check your level of cover, or contact us and we’ll check for you.
When you do look into what your level of cover is, it’s important to clarify some details of your chemotherapy treatment. You’ll be covered for chemotherapy if the hospital has an agreement with CBHS and admits you as a day patient. However, you won’t be able to claim for services delivered as an outpatient.
Your CBHS Hospital cover might also mean that, under our Hospital Substitute Treatment program, you could be eligible to receive chemotherapy at home. Your specialist can advise you on whether home treatment is a viable option for you.
With CBHS Hospital cover you may also be eligible for a home-based cancer support program. These programs can help improve your quality of life through support from psychologists, exercise physiologists and dietitians. All of these health professionals are experienced in dealing with the complex needs of people undergoing cancer treatment.
You can call our Member Care team on 1300 654 123 or email help@cbhs.com.au to find out more.
Reaching out for support and more information
This is a challenging time in your life, so it’s normal to seek more information and support on all the treatment options available to you. The Cancer Council produces a comprehensive guide to understanding chemotherapy and what to expect when you have treatment. You can download a copy here or call the Cancer Council on 13 11 20 for more information.
If you are also trying to cope with emotional health issues as a result of your diagnosis and treatment, speak with your GP for guidance and reach out to mental health organisations for more support. It’s vital to remember, you are not on this journey alone.
All information contained in this article is intended for general information purposes only. The information provided should not be relied upon as medical advice and does not supersede or replace a consultation with a suitably qualified healthcare professional.
Sources:
https://www.cosa.org.au/media/332739/cosa-position-statement-v3-oct2020-final.pdf
https://www.canceraustralia.gov.au/affected-cancer/what-cancer/cancer-australia-statistics
Health and wellbeing
programs & support
You Belong to More with CBHS Hospital cover:
- Greater choice over your health options including who treats you
- Get care at home with Hospital Substitute Treatment program
- Free health and wellbeing programs to support your health challenges
Live your healthiest, happiest life with CBHS Extras cover:
- Benefits for proactive health checks e.g. bone density tests, eye screenings
- Keep up your care with telehealth and digital options
- Save on dental and optical with CBHS Choice Network providers
